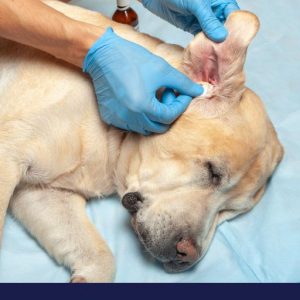
Essential Guide to Dog Skin Care
Your dog’s skin is more than just a protective layer—it’s a window into their overall health. From seasonal allergies to parasites, your dog’s skin can react to a variety of triggers. That’s why regular skin care isn’t just about grooming—it’s about preventing discomfort and catching problems early. […]

Beagles And Epilepsy
There are some dog breeds among which epilepsy is more prevalent than in the general population. […]

Finding Out About Joints And How They Can Affect Pets
The list of joint ailments in pets, particularly dogs and cats, is almost endless. You may have noticed some or all of these symptoms and wondered what could be causing the problem. […]

Skin Diseases: What To Watch For And Issues You Can Treat!
There are several skin diseases that can affect both cats and dogs and, unless severe, can be treated at home. […]

My Cat Has Inflammatory Bowel Disease: Can I Manage It At Home?
Inflammatory bowel disease (IBD) is a chronic condition that affects the gastrointestinal tract, particularly the intestines. […]

Dealing With Your Pet’s Upset Tummy And Diarrhea
If your cat is experiencing diarrhea, there are several steps you can take to help them. […]

Caring For Your Cat’s Ears
The most common ear problems in cats are infections generally caused by bacteria, yeast, fungus, or mite infestations. If an ear infection recurs, the causes should be identified and treated to prevent more severe complications in the future. […]

Stress In Pets And Digestion
Stress in pets is real and it can seriously affect how they are nourished. Chronic stress could lead to many negative outcomes with malnutrition and digestive disorders high on the list. […]

Gastrointestinal Health In Dogs And Cats
Any owner who has dealt with a pet’s sudden unexplained vomiting or diarrhea will understand that this is a stressful experience for everyone involved. […]

Your Cat’s Digestive System
Cats are known to be finicky eaters but understanding the basics of cat digestion can help you provide your pet with the nutrients they need. […]

Canine Eye Health
Dogs’ eyes, similar to those of most animals, have the same function and design as humans’ eyes. Both are thus subject to many of the same age-related changes and ailments. […]

Caring For Your Dog’s Skin
Most dog owners know that keeping your pet in great condition starts with proper nutrition. But after that, sensible skin care can also make the difference between your dog being happy or miserable. […]

Caring For Your Dog’s Ears
Ear infections, causing painful itchiness and irritation, are one of the most common problems afflicting dogs. Although ear infections themselves are problematic, there are usually underlying causes of the inflammation of the external ear canals that become inflamed with bacterial or yeast overgrowth. […]

Skin Cancer In Dogs
Skin cancer in dogs is far more common than most would expect. It accounts for approximately 30% to 40% of all cancer cases reported. […]

Cancer In Dogs
For any dog owner among the grimmest of news to get is that your beloved pet has been diagnosed with cancer. […]

Common Cat Diseases Pet Parents Should Know About
Find out which common cat diseases all pet parents should be familiar with. […]

Common Dog Diseases Pet Parents Should Know About
There are several common dog diseases all pet parents should be familiar with. […]

Dog Epilepsy Can Be Managed
Epilepsy in dogs is a common condition that cannot be cured, but it can be managed so your dog can have a full and happy life. Successful management requires lifelong medical attention and knowing what to do to best manage your dog’s condition. […]

Epilepsy In Dogs
Not everyone knows that dogs can suffer from epilepsy. Find out everything you need to know about epilepsy in dogs. […]

Discover The Causes Of Pain In Cats
What are the causes of pain in cats? Find out more. […]

What Causes Pain In Dogs?
Here’s an overview of things that can cause pain in dogs. […]

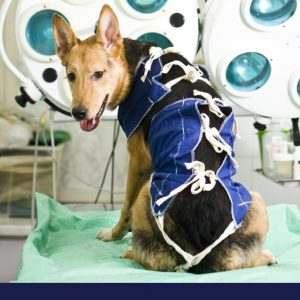
Things You Need To Know About Cat Surgery
Surgery is a scary word we don’t want to hear when it comes to loved ones, which include our feline friends, of course. […]

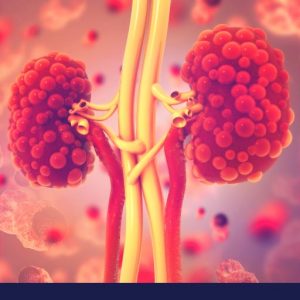
Acute And Chronic Feline Kidney Failure – How Long Can Your Cat Live?
Unfortunately, it is difficult to predict life expectancy with malfunctioning kidneys since each case is unique; however, there is a difference in life expectancy with regards to managed and unmanaged kidney failure. […]

CKD – The Silent Disease
The crucial functions of the kidneys include removing toxins and excess water from the body; maintaining water, salt and acid balance; producing hormones and maintaining normal blood pressure. […]

Stages Of Feline Chronic Kidney Disease
Chronic kidney disease is staged depending on the severity. This is estimated based on the level of waste products in the blood and abnormalities in the urine. […]

An Overview Of Feline Chronic Kidney Disease (CKD): Symptoms, Causes & Treatment
Early stage of chronic kidney disease (CKD) in cats is often unnoticed. Once you start noticing signs and symptoms, the disease is usually already in stage 2, late stage kidney insufficiency, or possibly stage 3, early kidney failure. […]
Kidney Toxicity (Drug Induced Nephrotoxicity) In Dogs
Like human kidneys, a dog’s kidneys balance certain substances in the blood and filter out and excrete the body’s waste as urine. Some drugs administered for the purpose of diagnosing or treating another medical disorder may have toxic effects on a dog’s kidneys. […]

Heart Disease In Dogs
Just like people, dogs can suffer from many of the same diseases, including heart disease (otherwise known as cardiomyopathy). […]

An Overview: Epilepsy & Seizures In Dogs
Seizure disorders in dogs are common and there are many causes which can include birth defects, metabolic defects, infections, a brain abscess, toxins or vascular disorders such as strokes and high blood pressure. […]

Rabies: Diagnosis, Prevention & The Value Of Vaccination
Rabies is a dangerous, fatal viral disease that can be contracted by animals and humans. Rabies is mainly transmitted by infected wildlife like bats. […]

What To Do During A Dog’s Seizure
There are often warning signs when a dog is about to have a seizure. A dog may begin to act scared, dazed, stressed or anxious without cause. Dogs may also have trouble seeing, experience muscle and limb contractions, and even lose bowel and bladder control. […]

World Rabies Day – Awareness & Prevention Efforts
Rabies spreads when the saliva of an infected animal – through a bite or otherwise – comes into contact with broken skin (which includes scabs) or the eyes, nose or mouth of another animal or person. World Rabies […]

Pet Diabetes
What is pet diabetes? How common is diabetes in pets? What signs should I look out for? How is diabetes diagnosed? How is diabetes managed in pets? […]

Canine Heart Disease Is Dangerous: What You Need To Know
Did you know that canine heart disease is just as dangerous in dogs as it is in people? […]

What You Need To Know About Zoonotic Diseases
A zoonotic disease (or zoonosis) is a type of disease that passes from an animal or insect to a human. […]

Diabetes Mellitus In Cats
Diabetes mellitus (DM) affects between 0.2% – 1% of cats in the general population. […]

Companion Animals and Coronavirus
There are various types of coronaviruses. This article looks at the differences between the two types you should know about. […]

The Management and Prevention of Diabetes in Cats
More and more cats are developing diabetes mellitus. Cat owners need to act on this alarming fact by learning more about this chronic disease. […]

CKD Risk Factors in Cats
A risk factor is defined as an attribute that is associated with increased risk of an outcome. However, the detection of risk factors for chronic kidney disease (CKD), which refers to the gradual decline of kidney function over time, is complicated because cats are often taken to the veterinarian when the disease is advanced. […]

The Importance of Catching and Diagnosing Diabetes in Cats Early
Unfortunately, diabetes cannot be cured. That’s why it’s very important to look out for signs of diabetes in cats so you can act early. A healthier and longer life is possible with treatment and proper management of the disease. […]

Treating Pain In Your Pet With NSAIDs
In recent years, the medical care of pain in pets has advanced rapidly. In veterinary medicine nonsteroidal anti-inflammatory drugs (NSAIDs) are approved analgesic medications designed to control pain and inflammation. […]

Pets In Pain Seldom Vocalize
Your pets can’t tell you where or how much it hurts but they suffer from pain just as we do. Animals have evolved to hide their pain as a protection against predators. […]

Is Your Dog Slowing Down Because Of Aging?
All dogs age differently but most dogs enter their senior years at about 7 years old (a little sooner for larger dogs) and begin to slow down and may gain weight more easily. An aging dog’s behavioural, mobility and temperamental changes will give you clues as to what they may need. […]

Post-Surgery Pain Management Is Critical
Surgery can be challenging for both pets and their owners. The recovery process is usually simple, but the first few days and weeks after surgery require special care for your pet. […]

Pain Can Be Predictable
There have been significant advances in veterinary medicine in understanding how pets feel pain. Veterinarians and their health care team are trained to recognize signs of a pet’s discomfort or fear. […]

Pain Can Be Controlled
If you notice changes in your pet’s behaviour or appearance, it could be because of pain. Pets usually hide their pain and cannot tell you where or how much it hurts. […]
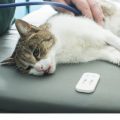
Faces of Pain
When we humans are in pain, we generally talk about it. Your dog or cat can’t tell you where or how much it hurts and usually mask their pain. Animals have evolved to withdraw and hide the signs of pain because any display would put them at risk with predators. […]

Health Issues & Conditions In Specific Dog Breeds
A big part of a dog’s general wellbeing is their health. Unfortunately some breeds are more likely to suffer from certain conditions than others. These breeds are: Bulldogs, Beagles & Boxers. However, they’re not the only ones. […]

Rabies: How It Spreads, The Signs & Why Vaccination Is Vital
Rabies is a zoonotic viral disease, meaning a disease that normally exists in domestic and wild animals that can infect humans. It attacks the central nervous system and once symptoms […]

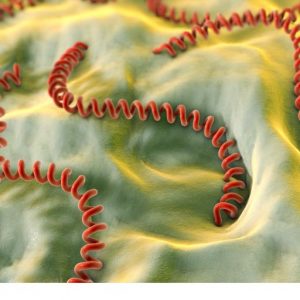
Leptospirosis – A Serious Bacterial Disease
Leptospirosis is an infectious disease caused by a type of bacteria called Leptospira. This bacterial disease can infect domestic animals, wildlife and humans. The disease causes fever, jaundice, kidney failure, abortion and may be fatal in severe cases. […]

Lyme Disease And Ticks
Ticks can transmit a number of diseases including Lyme disease and Rocky Mountain spotted fever, depending on the type of tick. […]

Rabies In Pets
Whenever you hear the word ‘rabies’ you should pay attention. Mammals – for our purposes humans, dogs and cats – can all get rabies. Rabies is a deadly virus and survival is […]

An Overview Of Cancer In Cats
It’s unclear what causes most cancers in cats. Fortunately for cat owners, feline cancer is not as common as cancer in dogs. Still, it’s good to be aware of the signs of cancer in cats because they can hide illness which can delay diagnosis and treatment. […]

An Overview Of Cancer Causes And Signs In Dogs
Better healthcare and improved nutrition have increased the average lifespan of canines. Unfortunately, with old age comes greater cancer risks. Still, any dog can develop cancer when an abnormal growth of cells occur […]

Stomach And Intestinal Cancer (Leiomyosarcoma) In Cats
Stomach and intestinal cancer is also known as leiomyosarcoma, which arises from the smooth muscles of the stomach and intestines. Leiomyosarcoma is an uncommon cancerous tumor that is an extremely serious and painful disease. […]

Pancreatic Cancer (Adenocarcinoma) In Dogs
What is Pancreatic Cancer (Adenocarcinoma) in Dogs? The pancreas is a gland organ in the digestive and endocrine systems. It is responsible for hormonal and digestive functions. Pancreatic cancer develops as abnormal pancreatic cells multiply rapidly in the pancreas. […]

Diagnosing, Treating & Preventing Cancer In Cats
It’s important to find and treat cancer in cats as early as possible because many types of tumours in cats tend to form, grow and spread quickly. With the appropriate treatment, long-term prognosis can be improved. […]
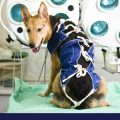
10 Common Canine Cancers: Part 1
Cancer is a complex disease that is unfortunately very common in both humans and dogs. It can be triggered by various things such as environmental, genetic and lifestyle factors. […]

10 Common Canine Cancers: Part 2
This is Part 2 of Common Canine Cancers: Read Part 1 first. […]

Types Of Rare Cancers In Cats
The following tumours and cancers are rare in cats. Some brain tumours start in the brain. They’re called primary tumours and are very rare. Secondary tumours on the other hand develop as a result of a different cancer that has spread to the brain. Brain tumour symptoms may include: […]

Diabetes In Cats: Symptoms
More and more cats are developing diabetes mellitus. Cat owners need to act on this alarming fact by learning more about this chronic disease. […]

Diabetes In Dogs: Symptoms
The occurrence of diabetes in canines is increasing. Find out what it is and what symptoms to watch for. […]

Diabetes In Cats
Feline diabetes, or diabetes mellitus, is a disease caused when the body cannot properly respond to the hormone insulin, which is produced and released by the pancreas. As in the human body, the cells in a cat’s body need energy in the form of glucose (sugar) for their […]

Diabetes In Dogs
Diabetes, or diabetes mellitus in dogs, is a chronic disease caused when the body cannot properly respond to the hormone insulin, which is produced and release by the pancreas. […]

The Importance Of Catching And Diagnosing Diabetes In Dogs Early
Diabetes, or diabetes mellitus in dogs, is a chronic disease caused when the body cannot properly respond to the hormone insulin, which is produced and release by the pancreas. […]

Management And Prevention Of Diabetes In Dogs
While diabetes in dogs may not be curable, it can be managed quite successfully. […]

Acid Or Gastroesophageal Reflux (GERD) In Cats
Cats, like humans, can suffer from acid or gastroesophageal reflux disease, GERD. Acid reflux is quite common in cats and while younger cats are at greater risk, cats of all ages may be susceptible. During a gastric reflux episode there is an uncontrollable reverse flow […]

Acid Or Gastroesophageal Reflux (GERD) In Dogs
Dogs, like humans, can suffer from acid or gastroesophageal reflux disease, GERD. Acid reflux is quite common in dogs and while puppies are at greater risk, dogs of all ages may be susceptible. During a gastric reflux episode there is an uncontrollable reverse flow of gastric […]

Constipation In Cats
Constipation is the inability to routinely and easily evacuate the bowels resulting in retention of feces or passage of hard, dry feces. When a cat is constipated, the colon—the section of the lower intestine that contains undigested food, mucus, bacteria, and dead cells before elimination—has become impacted with […]

Constipation In Dogs
Constipation is the inability to routinely and easily evacuate the bowels resulting in retention of feces or passage of hard, dry feces. When a dog is constipated, the colon—the section of the lower intestine that contains undigested food, mucus, bacteria, and dead cells before elimination—has become impacted with […]

Acute Diarrhea In Cats
Cats with acute diarrhea may defecate more frequently, and may have softer, looser or more watery feces. Blood, mucus, or even parasites may be visible in or on their stools and they may have accidents in the house. Diarrhea is quite common and is brought on by […]

Acute Diarrhea In Dogs
Dogs with acute diarrhea may defecate more frequently, and may have softer, looser or more watery feces. Blood, mucus, or even parasites may be visible in or on their stools and they may have accidents in the house. Diarrhea is quite common and is brought on by […]

Ear Infections In Cats: Signs, Causes, Diagnosis, Treatment & Prevention
Luckily, when it comes to ear infections, cats are not as vulnerable as dogs. Still, when they do get them, the effects can be painful and even cause damage if left untreated. Signs and Symptoms of Ear Infections in Cats […]
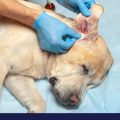
Ear Infections In Dogs: Treatment & Prevention
If your dog has an ear infection, it’s really important to approach the problem properly. The safest and smartest first step would be to contact your vet. […]

Ear Infections In Dogs: Signs, Causes & Diagnosis
The first thing you should know is that ear infections in dogs are quite common. The important thing is to address signs and symptoms as soon as you notice them. […]

Ear Infections In Cats
Ear infections, causing painful itchiness and irritation, are not as common in cats as they are in dogs. Although ear infections themselves are problematic, there can be underlying causes of the inflammation of the external ear canals that become inflamed. If your cat gets an ear […]

Chronic Ear Infections In Dogs
Ear infections, causing painful itchiness and irritation, are one of the most common problems afflicting dogs. Although ear infections themselves are problematic, there are usually underlying causes of the inflammation of the external ear canals that become inflamed with bacterial or yeast overgrowth. With overgrowth of […]

What You Should Know About Epilepsy In Cats
Just because it’s more common for dogs than cats to suffer from epilepsy doesn’t mean epilepsy in cats should be taken lightly. Before we get to symptoms, causes and treatment it’s important to understand the difference between a seizure and epilepsy. […]

What You Should Know About Seizures In Dogs
Epilepsy is a brain disorder that is more common in dogs than in cats. It’s also important to know that a seizure is a single occurrence while the word epilepsy is used when two or more unprovoked seizures have occurred. […]

A List Of Common Eye Conditions In Felines
Cats have very unique and beautiful eyes. They can detect much more light than we can, however, their colour vision is limited. Threats to healthy eyes include injuries, conditions and diseases. […]

A List Of Common Eye Conditions In Canines: Part 1
Dogs’ eyes are very important organs that help them form images of the world. Threats to healthy eyes include injuries, conditions and diseases. […]

A List Of Common Eye Conditions In Canines: Part 2
Welcome to Part 2 of common eye conditions in canines. […]

Facts About Your Cat’s Eyes
Cats are weird, wonderful and rumoured to be wise… especially when you look in their eyes! But, how do they actually view the world around them? Well, science has come up with a few generally agreed upon facts to help us understand this interesting feline organ. […]

Eye Inflammation (Anterior Uveitis) In Cats
Uveitis is one of the most common eye disorders in cats and can be extremely serious. Without medical attention, your cat’s eyesight is at great risk. Uveitis is inflammation of the uvea, which is the dark tissue at the […]

Heart Disease In Cats
We don’t want to know or think about it, but cats, just like people, can also suffer from heart disease. Any disease that affects the heart muscle is called cardiomyopathy and can lead to heart failure. Cardiomyopathies are classified according to the effect they have on the heart […]

Facts About A Dog’s Heart
Studies show that people who own pets are healthier, have fewer heart attacks and live longer. Happy, healthy dogs also live longer than unhealthy, unhappy dogs. Still, just like human, dogs can suffer from heart problems too. […]

Facts About A Cat’s Heart
The body needs oxygen-rich blood. The heart makes sure this blood gets around. Then, once the oxygen-depleted blood goes through the lung fields, the cycle repeats. A cat’s heart is a small yet impressive organ which works around the clock. In fact, their little hearts beat like crazy, which is surprising, since cats seem calm and confident most of the time. […]

Enlarged Heart (Dilated Cardiomyopathy) In Cats
Did you know that feline heart disease is just as dangerous in cats as it is in people? What is an enlarged heart? The heart has four chambers: two chambers at the top, the right and left atrium; and two chambers at the bottom, the […]

CKD A Common Disease In Domestic Cats
Chronic kidney disease (CKD) is a common, progressive and debilitating disease in cats, affecting a large number of cats crossing consulting room tables in veterinary clinics. The prevalence of feline CKD increases with age. Geriatric cats in general often develop some degree of kidney disease. […]

Causes Of Feline Chronic Kidney Disease
An Overview of the Function of the Kidneys. Chronic kidney disease (CKD) is a common problem in cats. Kidneys are essential for normal bodily functions. […]

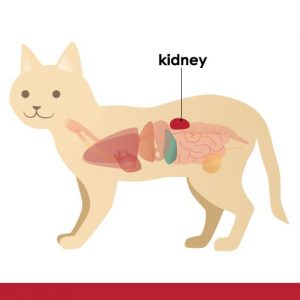
Feline Kidneys: The Facts
Feline kidneys are paired organs that reside in the dorsal abdomen. One is situated on the left and the other on the right. The kidneys at birth are the same kidneys for the rest of a cat’s life. […]

What To Do When Your Cat Is Diagnosed With CKD
Following blood and urine tests, X-rays, an ultrasound, or biopsy, your veterinarian may give you the diagnosis that your cat has chronic kidney disease (CKD). […]

Chronic Kidney Disease In Cats – About The Disease
CKD affects approximately 35% of geriatric cats and up to 10% of cats that visit veterinary clinics. The disease is progressive over time and occurs where there is long-standing, irreversible damage to the kidneys that weakens their ability to remove waste products from the blood and regulate other essential functions. […]
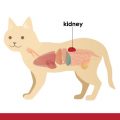
Feline Kidney Problems
This article takes a look at how kidneys work and what stops them from doing their job. […]

Chronic Kidney Disease In Cats – Signs, Prognosis, Management
Chronic kidney disease (CKD) is the name used to refer to cats with kidney failure (or chronic kidney failure). CKD is most common in middle to old-aged cats. Since it is a progressive disease there is a gradual decline and worsening of the condition. […]

Chronic Kidney Disease And Its Complications
Chronic kidney disease (CKD) is defined as a progressive irreversible deterioration of kidney function or structure in one or both kidneys that has been continuously present for 2 months or longer. […]

Management Of CKD In Cats
Chronic kidney disease (CKD), or a slow decline in kidney function over time, is common in cats. Filtering the blood and making urine are the most important functions of healthy kidneys. […]

Kidney Failure In Cats
Chronic kidney disease (CKD) requires lifelong treatment and can be challenging for both the cat and its human family. […]

Chronic Kidney Disease Is Irreversible & Incurable
Chronic kidney disease (CKD) requires lifelong treatment and can be challenging for both the cat and its human family. […]

A Guide To Chronic Kidney Disease In Cats
Chronic kidney disease (CKD) is one of the two main kidney diseases that can affect cats. CKD is usually caused by long-term diseases that slowly damage the kidneys and reduce their function over time. […]

Management Of Feline Chronic Kidney Disease
A cat’s kidneys are very important for the functioning of the body. Kidneys do a variety of things, such as: helping to manage blood pressure, making hormones, stimulating the bone marrow to make more red blood cells, removing waste from the blood. […]

Importance Of Nutrition In Chronic Kidney Disease In Cats
The kidneys have many functions. Two of the major functions include removing waste products from the blood and conserving water in the body. With kidney disease the kidney function declines and toxic waste products like urea and phosphorous begin to build up in the body. […]

Management Of Cats Living With CKD
Chronic kidney disease (CKD) requires lifelong treatment and can be challenging for both the cat and its human family. […]

Nutrition For Cats With CKD
With treatment and careful management, cats with Chronic Kidney Disease (CKD) can have a good quality of life. […]

Dietary Management In Cats With CKD
Several studies have shown that dietary management plays a key role in cats with chronic kidney disease (CKD) which is a common and unfortunately incurable condition. CKD is actually more than just a common progressive condition, it is a leading cause of death in cats, often due to the complications it causes. […]

What Is Osteoarthritis?
Arthritis is a general medical term describing inflammation of the joints. Osteoarthritis (OA) or degenerative joint disease (DJD) is the terminology used when referring to a form of chronic joint inflammation that is a progressive and permanent disease of joints. […]

Osteoarthritis In Dogs
Dogs, just like humans, can also suffer from osteoarthritis (OA), sometimes called degenerative joint disease. […]

Osteoarthritis In Cats
Cats are natural survivors and masters at hiding pain, which means discomfort and illness often go unnoticed. If owners and veterinarians can’t see any issues, no diagnosis can be made which means symptoms and pain caused by diseases go untreated. […]

What You Should Know About Osteoarthritis
Since dogs cannot easily tell us that they are in pain and signs may be subtle, it’s difficult to identify pain. There are many misunderstandings regarding pain in animals. […]

An Overview Of A Dog’s Joints & Ligaments
Joints are found throughout the body wherever two bones meet. A joint is formed when two bones come together and are held in place by supporting tissues. […]

What Are The Signs & Symptoms Of Pain In Dogs?
Pain in dogs is a tricky thing, because it’s not always so obvious … until it’s more severe. So, as pet owners we should educate ourselves about the signs and symptoms of pain in dogs so that we can provide relief as soon as possible. […]

Signs That Could Mean Your Cat Is In Pain
Pain in cats is a tricky thing because it’s rarely obvious… until it’s quite severe. Cat owners should therefore educate themselves about the signs and symptoms of pain in cats so they can offer relief as soon as possible. […]

Pain Management For Your Dog
Like humans, dogs are happier when they are healthy and pain-free. The thing is, it’s not always obvious when a dog is experiencing discomfort. It’s up to dog owners to learn about signs and symptoms of pain […]

What Are NSAIDs For Pets And How Do They Work?
The term NSAIDs stands for nonsteroidal anti-inflammatory drugs. They are often used to relieve pain and inflammation – in people and animals. However, animals should not be given NSAIDs created for humans. […]

Possible Side Effects Of NSAIDs And Safety Of Long-Term Use
If you’re a pet owner, it’s important to educate yourself about nonsteroidal anti-inflammatory drugs (NSAIDs) in case your pet needs them someday. […]

How To Manage Pain In Dogs
You need to contact your veterinarian as soon as you notice signs and symptoms of pain in your dog. A veterinarian can investigate to determine the cause of pain and recommend treatment to offer relief. […]

Surprising Facts About NSAIDs Pet Owners Should Know About
Sometimes our pets need medication because they’re sick, for example, they may be experiencing temporary digestive problems. Other times they may need medication for pain caused by injury or a chronic condition. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help with the last-mentioned situation. […]

Information For Owners Whose Dogs Are On NSAIDs
If your dog needs to start taking NSAIDs, it’s important to get a Client Information Sheet from your veterinarian. This valuable resource will guide you and be handy anytime you need to check instructions or other important details. […]

A List Of Common Skin Problems In Cats
Common skin problems you should be aware of. […]

What’s Causing Your Dog’s Skin Problems?
Nobody likes having an itchy or irritated skin and your dog is no different. Unfortunately, skin problems are very common in canines and shouldn’t be ignored. Fortunately, most causes of skin problems in dogs are not difficult to address and treat. Some can even be prevented. […]

Abscesses In Cats
A common skin condition in cats is an abscess that can form if an irritation worsens or if bacteria invades the skin. An abscess can be quite unsightly and alarming and can be found on almost any part of a cat’s body. Whether small or large, abscesses will […]

Abscesses In Dogs
A common skin condition in dogs is an abscess that can form if an irritation worsens or if bacteria invades the skin. An abscess can be quite unsightly and alarming and can be found on almost any part of a dog’s body. Whether small or large, abscesses will […]

An Overview Of Stud Tail In Cats
If you haven’t heard of stud tail in cats, or want to know more, here’s a handy overview. […]

The Causes And Signs Of Yeast Infection In Dogs
Yeasts are microscopic fungi. Opportunistic fungi can increase and cause skin, paw and ear infections when the circumstances are right. The condition can be super uncomfortable and should be addressed as soon as possible before it gets worse. […]

What You Should Know About NSAIDs For Dogs
Pain can significantly affect the physical and emotional well-being of dogs. However, when pain is reduced and carefully managed, dogs can lead happier, more comfortable lives. […]

Anemia Due To Iron Deficiency In Cats
Anemia is not a specific disease and doesn’t present in isolation, but is a symptom or condition that occurs as a result of other processes going on. When a cat has anemia there is a drop in the number of red blood cells […]

Anemia Due To Iron Deficiency In Dogs
Anemia is not a specific disease and doesn’t present in isolation but is a symptom or condition that occurs as a result of other processes going on. When a dog has anemia there is a drop in the number of red blood cells in […]

Cat Anxiety
As in humans, stress and anxiety in cats can impair the ability to function and further aggravate existing physical conditions. Any change in a cat’s environment can cause stress and anxiety. Environmental changes are often the cause and emotional stress is the effect. […]

Anxiety In Dogs – Fears & Phobias
Anxiety or fear is the feeling that something bad or unpleasant will happen. It is related to uneasiness, nervousness, restlessness, tension and dread. When it feels like a situation, person or object is posing a threat, whether real or believed, an instinctual anxiety can be […]

Upper Respiratory Infections In Cats
A cat’s respiratory system consists of the large and small airways and the lungs. As a cat breathes air in through its nose or mouth, the air travels down the trachea, which divides into the tubes known as […]

Aspiration (Or Inhalation) Pneumonia In Dogs
Dog owners need to be aware of the risk of aspiration (or inhalation) pneumonia. What is aspiration (or inhalation) pneumonia? Aspiration pneumonia, also called inhalation pneumonia, occurs when a dog’s lungs become inflamed […]

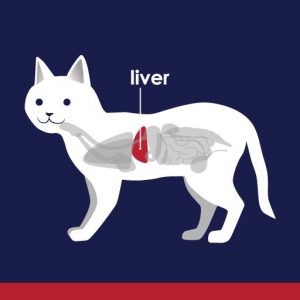
Facts About Your Cat’s Liver
To understand how a cat’s liver works and what it does, you have to know a little bit about its structure and location. Placement and Abilities. The liver sits behind the diaphragm and in front of the stomach, slightly more to the right side.[…]

Stress In Dogs
Dogs, like humans, can experience chronic stress causing a variety of physical issues that can develop into serious health problems. Prolonged stress may also affect a dog’s emotional state making him more aggressive or potentially dangerous. Stress or anxiety are more common in dogs than we think. […]